Computational Health Informatics lab research
Research
This page outlines general research themes at the CHI Lab, which are in a constant state of evolution, and which therefore vary from month to month, in response to the needs of our collaborators.
Acute and Critical Care

The Intensive Care Unit (ICU) represents the highest level of acuity within the hospital system. After discharge from the ICU, patients are sent to recover on "step-down wards" or "high-dependency units". While on these acute wards, there is a substantial risk of avoidable deterioration in the patient's condition. Adverse outcomes of this kind are approximately similar in number to the annual mortality due to road-traffic accidents, and represent one of the largest sources of avoidable death in modern healthcare systems.
Our on-going projects in acute care, in collaboration with world-leading intensive care clinicians at Oxford University Hospitals, aim to produce predictive AI-based systems using the huge quantities of data now routinely collected for each patient. Other outcomes from this theme of research include predictive systems to better improve the operation of the hospital, including predictively allocating beds and tests for patients.
Infectious Disease
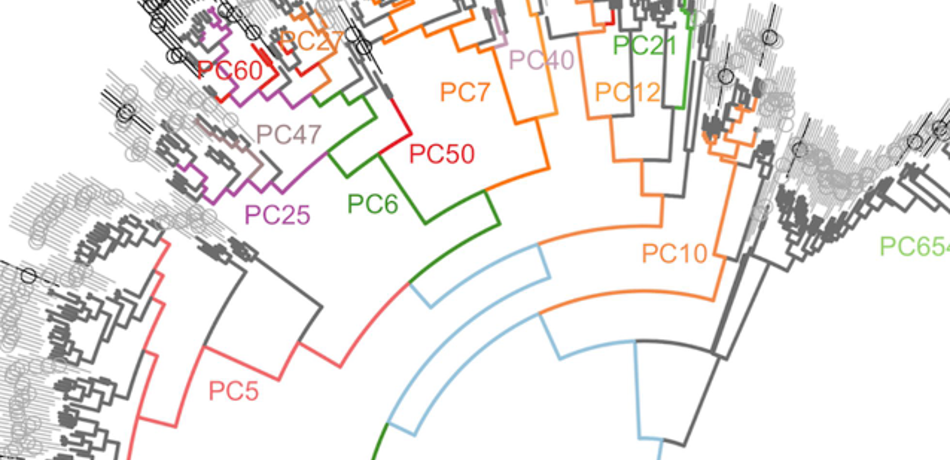
The UK Chief Medical Officer noted that "infectious disease is as great a threat to national security as climate change, with more than one new threatening disease identified each year", and that "the difficulty and challenge in identifying and tracking future threats is not the acquisition of trusted physiological and genomic data, but in using these huge databases with new computer science methods for analysis."
We use machine learning to greatly improve our ability to identify and fight outbreaks of infectious disease - including the COVID-19 pandemic of 2020 - using AI-based systems. This theme of research collaborates closely with the UK Health Security Agency (the UK's Centre for Disease Control), experts in microbiology from Oxford University Hospitals, and a global network of CDCs from some of the world's largest countries. We also work closely with the Oxford Vaccine Group for developing and evaluating vaccines to fight infectious disease.
Our work in this wide-ranging area falls within Oxford's new Pandemic Sciences Institute, for which CHI Lab provides the AI research theme.
Wearables

The overwhelming majority of ambulatory patients in modern healthcare systems are monitored only manually, by members of the clinical staff. There is an urgent need for mobile ("m-health") systems, comprising unobstrusive patient-worn sensors and lightweight processing (such as via smartphone) that are sufficiently robust for use in clinical practice.
CHI Lab is actively researching (i) the tracking of vital signs from sensors in a robust manner; (ii) performing intelligent processing of the resulting data to stratify patients according to risk; and (iii) working on forecasting methods for predicting serious physiological events. These collaborative projects include applications in Oxford University Hospitals and with university spin-outs.
Complex Disease

Major CHI Lab projects focus on the development of AI-based systems to exploit rich clinical datasets, with the goal of improving the understand and treatment of complex diseases. The Oxford University Hospitals and wider collaborations provide very great opportunities to develop new AI methods for diseases that often include both genomic and clinical data.
We have large on-going EPSRC- and Wellcome-funded activity in cardiovascular disease and ECG analysis; chronic obstructive pulmonary disease (COPD, or lung disease); epidemiology via the UK Biobank and China Kadoorie Biobank; and immune disease. All of these projects are characterised by the needs of complex methods to link the very many different types of data that are typically available for each disease.
Low- and Middle-Income Settings

This theme includes a number of initiatives that seek to improve access to healthcare in low- and middle-income countries (LMICs). Using AI-based algorithms within smartphones and wearables, we are able to use inexpensive sensors that are appropriate for use at scale in LMICs. The delivery of healthcare in such settings is often performed by healthcare workers without high levels of clinical training, and so there is therefore a need for the decision-support capabilities of such algorithms.
This work builds on the Wellcome Trust's first "Flagship Innovation Centre", which joins CHI Lab in Oxford to the Oxford University Clinical Research Unit in Vietnam; the goal of this major programme is to develop innovations for improving access to healthcare in south-east Asia and beyond. We also work closely with experts in overseas development at the School of Geography & the Environment at Oxford to deliver technology-based systems for improving water security in LMICs.


