03 May 2021
Multi-partner 'OpenMind' consortium to develop technology for new generation of neurostimulation devices
The new consortium is led by UCSF and funded by a $4.4 million NIH grant from the NIH BRAIN Initiative
Investigators at the University of Oxford, University of California San Francisco (UCSF), Brown University and the Mayo Clinic have joined forces to develop open-source technology platforms for a new generation of neurostimulation devices that not only provide stimulation to the brain but also sense, record, and stream brain activity.
The new ‘OpenMind’ consortium is led by UCSF and funded by a $4.4 million NIH grant from the NIH BRAIN Initiative. One of the major objectives of the BRAIN Initiative is to make new technology widely available to help people affected by neurologic and neuropsychiatric disorders.
Dr Philip Starr, principal investigator and neurosurgeon at UCSF, said: ‘These four groups have been the earliest investigators to work on these advanced new neurostimulation devices and together bring the highest levels of expertise in this field.’
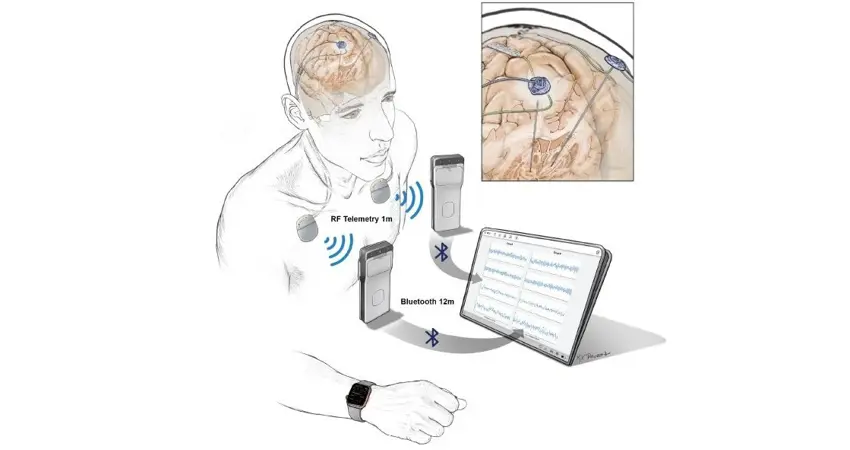
Traditional stimulation devices to treat neurological disorders like Parkinson’s disease provide constant electrical stimulation to the brain in an effort to disrupt aberrant neural circuits that lead to symptoms. The new generation of devices provide stimulation, but for the first time also have the ability to record brain signals and stream high volumes of that data outside the lab as patients go about their normal activities in the real world.
Dr John Ngai, director of the NIH BRAIN Initiative, said: ‘As we move toward modulating brain circuitry in real-time, the increasing complexity of the technology requires collaboration among neuroscientists, computer scientists, and engineers to develop safe and effective interventions that also adhere to neuroethical principles.’
By correlating these data with patients’ symptoms, investigators hope to better understand the neural circuits underlying brain disorders - ranging from epilepsy and movement disorders to severe psychiatric disorders - and develop personalized, intelligent therapies to normalize circuits that have gone awry. This would not only avoid side effects associated with constant stimulation, but allow for a therapy tailored to an individual patient.
While representing enormous potential for better treatment of many poorly understood brain disorders the new devices are also technologically complex, imposing significant barriers to use by researchers.
Dr Starr said: ‘Part of the reason the device is so flexible and tailorable is that the investigators write the software that controls it, which is something only device companies have been doing in the past. We also are therefore responsible for documenting that the device works according to FDA regulations.’
Writing custom software for the device is not only costly and time-consuming, but requires specific knowledge regarding security and quality controls. All of these are necessary for safety, but also pose hurdles to technological development in academic settings, and led to a growing awareness at the NIH of the need for a consortium of experts to help disseminate enabling technology resources.
Professor Tim Denison, Royal Academy of Engineering Chair in Emerging Technologies, who is leading the Oxford contribution from the Department of Engineering Science and MRC Brain Network Dynamics Unit, said: 'The OpenMind consortium is developing critical tools for foundational clinical neuroscience and therapy development that leverage the latest medical devices. These devices can be applied for exciting discovery, but also require careful consideration of subject safety and regulatory requirements. Oxford’s role is to help develop and pilot an ‘open source quality management system’ that allows academics to develop safe and reliable software for investigational studies, and share best practices among protocols.'
One of the goals for the Open Mind Consortium is to leverage the best tools and ensure that they are made available as quickly as possible. These include best-practice guidance and generalizable software applications that can be upgraded as the current devices phase out and new versions come to market.
The group aims to not only disseminate tools and technologies that can be used by the wider research community, but also work with the NIH and manufacturers to develop standards on software architecture, security features, data sharing, and neuroethics for others applying for grants that use these new devices.
A Steering Committee that includes neuroethicists and patient advocates will also advise on the development of these standards as they relate to patient consent and control of the device and streaming.
By creating a common technical and regulatory infrastructure for the devices, Open Mind ultimately aims to create a more streamlined regulatory pathway for FDA approval of investigational protocols. Denison added, “while the focus of the NIH-funded OpenMind consortium is on FDA regulations, the Oxford team is also adapting these methods for MHRA requirements to enable research collaborations with UK-based manufacturers, in applications ranging from deep brain stimulation to transcranial magnetic stimulation.”
Read the Nature Biotechnology paper online




